This document has been produced by ORPHANET working jointly with the CADASIL France association and CERVCO.
Source: CADASIL, Encyclopédie Orphanet Grand Public, avril 2008
http://www.orpha.net/data/patho/Pub/fr/CADASIL-FRfrPub1001v01.pdf
What is CADASIL?
CADASIL is a genetic disease affecting the small blood vessels in the brain. It leads to poor blood supply to certain areas of the brain, causing symptoms that vary greatly from one patient to another. The commonest signs of the disease, which appear in adulthood, are migraine, psychic disorders and stroke which can affect language, memory, vision etc.
The term CADASIL was suggested in 1993 by French researchers as the name of the disease. It is an acronym which, in English, stands for « Cerebral Autosomal Dominant Arteriopathy with Subcortical Infarcts and Leukoencephalopathy ».
The term "cerebral arteriopathy" means that the arteries in the brain are affected. These are the vessels which carry the blood to all the organs in the body.
"Autosomal dominant" describes the way in which the disease is passed from one generation to the next, since this is a hereditary illness.
The term "infarct" means the sudden cessation of blood circulation in one part of the body which, in the case of CADASIL, is the "sub-cortex", one of the regions in the brain.
Finally, the word "leukoencephalopathy" refers to lesions in the brain caused by the disease (see below).
How many people suffer from this disease?
The prevalence of CADASIL (i.e. the number of people affected within a population at any given moment) is not known exactly but it is estimated to be 1 in 24,000. However, this prevalence is probably an underestimation.
Who can be affected? Is it present all over France and the world?
The disease affects as many men as women. The symptoms appear in adulthood, usually between the ages of 30 and 40.
Although initially described in Europe, CADASIL has since been observed in populations from very different backgrounds, all over the world.
What causes the disease?
The disease is caused by an abnormality (a mutation) in a gene called NOTCH3.
This is an important gene during foetal development, controlling blood vessel formation and, to be more precise, the formation of the muscle layer which is a part of the arteries.
Because of the abnormality in the Notch3 gene, the muscle layer in the arteries is of poor quality and it is gradually damaged. The walls of the arteries become less elastic and blood circulation is more difficult.
Although it affects the small arteries in all the organs of the body, the consequences of the disease are only apparent in the brain, leading to the neurological problems described below.
Certain areas of the brain, which are irrigated by small arteries, are deprived of a blood supply and, therefore, of oxygen by the abnormality in the small arteries. This is what we call an "infarct". Oxygen is essential for cell function and survival and the repetition of small infarcts in part of the brain cause the initial symptoms and gradually cause them to worsen.
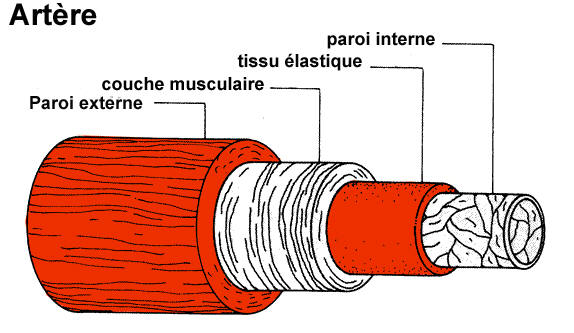
Figure 1
An artery is a sort of flexible tube consisting of several concentric layers or "tunics". One of them is a solid, elastic layer of muscle that maintains the diameterof the artery and enables the blood to circulate. The Notch3 gene plays a part in the development of this muscle layer.
(http://www.ulb.ac.be/erasme/edu/fcc/hypertension/images/sch_artere_400.gif)
Is this a contagious disease?
No, CADASIL is not a contagious disease; it is a hereditary genetic disease.
What are the signs of the disease?
The disease is caused by an abnormality in the arteries and is present at birth but the first symptoms do not generally appear until adulthood (around 30 or 40 years of age). The symptoms vary greatly from one person to another, even within the same family (even though they all have the same genetic abnormality). Not everybody has all the signs described below. Likewise, the severity of the symptoms and, therefore, of the handicap resulting from the disease is unpredictable and very variable.
Migraine
Attacks of migraine with aura are frequent with this disease and are often the first symptom. Migraines are severe headaches (usually on one side of the head only), sometimes accompanied by nausea, vomiting and an inability to tolerate noise and light (patients need to lie in a silent, dark room). These headaches can occur on their own but they are often preceded by abnormal feelings called "aura". Migraines with aura affect approximately one patient in four. The frequency of the attacks of migraine with aura varies greatly, ranging from two per week to one every three or four years.
The signs preceding a migraine, the "auras", differ from one patient to another. They usually last for 20 to 30 minutes, followed by the headache. They usually affect vision and may consist of dazzling "floaters" passing across the field of vision, coloured spots, the sudden appearance of a bright light in the centre of the field of vision (scintillating scotoma) or, more uncommonly, blurred vision or loss of vision in one half of the field of vision (hemianopia).
Other signs may affect the body's sensitivity with numbness, tingling, tickling, muscle weakness or even paralysis on one side of the body. These sensations can sometimes spread throughout the body.
Speech difficulties may also appear, often in the form of difficulty in finding words (aphasia) or in pronouncing them. The aura can also consist of a feeling of depression, anxiety or agitation.
Patients can also suffer from migraine without aura. However, this type of migraine is not more frequent in CADASIL patients than in the general population.
Migraines attacks can be extremely painful, sometimes unbearable, and can last for several hours or even for several days. In some cases, the attack is so severe that it requires hospitalisation for the patient.
Stroke
Stroke occur during this disease when an area of the brain is suddenly deprived of blood supply (infarction or ischaemia). Repeated brain infarctions are the most frequent complication of the disease, affecting more than three out of four patients. They usually occur between the ages of 40 and 50.
They can cause various symptoms, all of which occur suddenly e.g. paralysis of one side of the body (hemiplegia) or loss of feeling in one part of the body, speech difficulties, loss of balance or lack of coordination in movements.
These difficulties may regress in less than 24 hours but they may also become permanent as the disease develops. When they are "temporary", they are called transient ischemic attacks (TIA); if the difficulties are irreversible, they are called brain infarction.
Psychiatric and cognitive disorders
Mood alterations occur in approximately 20% of cases, either after a brain infarction or at any time during the progress of the disease. Certain patients show signs of major depression and a loss of motivation and interest in their work, leisure activities, plans for the future etc. (apathy). In rare cases, phases of depression alternate with phases of hyperactivity (excessive expenses, unusual remarks or behaviour patterns, a range of excesses etc.). They are described as suffering from bipolar disorders. The existence of these psychiatric disorders may lead to diagnostic errors, especially when they are the first signs of the disease.
So-called "cognitive" difficulties may also occur, from the onset of the disease. However, they do not become significant until the ages of 50 to 60. They consist of difficulties with concentration, a shortened attention span, or memory difficulties and vary in severity. People who are affected in this way often find it difficult to organise activity, plan something or take initiative. They also find it difficult to adapt to new situations and manage the changes that occur in everyday life. This affects executive functions (organisation, planning) and leads to a loss of mental flexibility.
Development of dementia
With age, the intellectual decline may become worse, either gradually or in stages (sudden, major worsening). Attention and memory difficulties increase, as does the loss of initiative. The worsening of these difficulties may lead to a loss of independence, a condition referred to as dementia or dementia syndrome.
Dementia is observed in one-third of all patients but its frequency increases with age. After the age of 60, some 60% of patients suffer from dementia, possibly associated with other signs such as difficulties with walking, urinary incontinence and, in certain cases, difficulties swallowing.
Epilepsy
In less than 10% of cases, patients also have epileptic seizure of various types (movements or convulsions including muscle spasm, tremor and stiffness), sensory disturbance (tingling, numbness, auditory or visual hallucinations i.e. hearing sounds or seeing things that are not there, etc.), psychic difficulties (panic attacks or panic-based fear, memory loss, confusion, loss of consciousness, absences _sudden loss of contact with the environment of which the patient has no memories afterwards, or excessive salivation, urinary incontinence etc. The fits can affect the entire body (general seizure) or, more often, a limited part or one-half of the body (partial seizure).
Why do the symptoms occur?
The loss of oxygen because of poor blood supply damage certain areas of the brain, creating lesions. After a few minutes without a blood supply, certain cells are peamanently destroyed. To be more precise, it is the "white matter" in the brain which suffers most often during this disease. This is why we use the term "leukoencephalopathy" ("leuko" means "white" in Greek). The white matter consists of bundles of "cables" known as axons, which are extensions of the nerve cells, or neurones (fgure 2). These "cables" are covered in an insulating sheath called "myeline", similar to the insulation that covers electrical wires.
Myeline helps to transmit the nerve message that operates in the brain. In people with CADASIL who suffer repeated minor infarcts or micro-haemorrhages, the myeline is altered or even destroyed (this is called "demyelination) in certain areas of the brain. The alteration damages or prevents the transmission of nerve messages in the brain and this is what causes a gradual loss of independence.
Figure 2
The nerve cells are extended by "axones" covered with a white myeline sheath. It is the axones, which "wire" the brain, that make up the white matter in which lesions are formed during CADASIL. (http://www.medisite.fr/medisite/Aquelles-lesions-anatomiques.html)
Breaks in the blood circulation seem to be increasingly frequent and severe as the disease progresses, which explain the gradual build-up of cerebral lesions and the worsening of symptoms. Once a lesion forms in the brain, it is permanent but other circuits may be built up to compensate for this loss, enabling the person to recover the functions lost. However, such an ability decreases gradually and the difficulties then become increasingly obvious.
The reason for which some people develop a more severe form of the disease is unknown.
How does the disease develop?
In most cases, the onset of the disease is marked by the appearance of migraine with or without aura after the age of 30 then the occurrence of stroke some ten or twenty years later and by the gradual onset of cognitive difficulties (problems with concentration, memory loss etc.) and difficulties with balance and walking at about the age of 60. After 60 years of age, the loss of independence and intellectual decline can be significant.
However, the severity of the disease varies greatly from one person to another, even within the same family. The disease develops more or less quickly. Some patients are seriously handicapped very early on, at about the age of 40, while others do not have the first symptoms of the disease until they have passed the age of 70.
Diagnosis
How is CADASIL diagnosed? What additional tests are required? Why are they done?
Diagnosis of the disease is initially based on magnetic resonance imaging (MRI). This is a painless examination in which the patient is placed in a device that produces a magnetic field. This then gives precise images of the brain. MRI diagnosis is completed by genetic testing.
In the case of CADASIL, the MRI detects lesions that are characteristic of the disease in the white cerebral matter (figure 3). The lesions usually appear between the ages of 20 and 35 but they may be present for many years without causing any symptoms. After the age of 35, all carriers of the abnormal Notch3 gene have abnormalities visible on an MRI scan and indicative of CADASIL, whether or not they have any symptoms. The number and extent of the abnormalities detected by an MRI scan increase with age.
In very rare cases, a skin biopsy is carried out to help in the confirmation of the diagnosis. This is a small sample taken under local anaesthetic, used to study the condition of the small blood vessels in the skin. Even if CADASIL is not causing any neurological symptoms, abnormalities in small arteries are visible all over the body, especially in the skin.
The CADASIL diagnosis is confirmed by taking a blood sample and looking for abnormalities in the Notch3 gene. This search requires specific management and follow-up.
Is it possible to mistake other diseases for CADASIL? Which ones? How can you differentiate between them?
Strokes are relatively common in the population as a whole and more particularly among the elderly, diabetics, hypertensives, smokers and people with high cholesterol. CADASIL is not therefore discussed when the first symptoms of stroke arise. However, the detection of typical lesions in the brain through the use of MRI scanning can alert the practitioner to the existence of a specific disease. When other cases have already been diagnosed in the family, it is easier to diagnose CADASIL but MRI scanning and genetic testing remain necessary to confirm the diagnosis since the neurological symptoms may be due to other diseases. Among the "similar" diseases are multiple sclerosis progressive multifocal leukoencephalopathy, cerebral amyloid angiopathy and Alzheimer's disease
Genetic aspects
What are the risks of transmission to children? What are the risks for other members of the family?
CADASIL is a hereditary familial disease. Its transmission is autosomal dominant, which means that a person already affected by the disease has a 1 in 2 chance of passing the abnormal gene on to his or her children (Figure 4). All the people who have inherited the abnormal gene will develop symptoms of the disease at some time or another. However, the severity may vary considerably from one person to another, even within the same family.
In a few known exceptional cases, the mutation of the Notch3 gene has occurred "randomly" ("de novo mutation"), without having been transmitted by one of the parents.
Can the disease be detected in people at risk before any symptoms appear?
It is possible to do a screening test before the appearance of any symptoms of the disease, in the members of a patient's family (presymptomatic testing). The test will show whether a person has the genetic abnormality and, therefore, whether he or she will develop the disease one day.
However, in a person with no sign of the disease, genetic testing will only be offered as part of a specialist consultation and precise medical and psychological management. No test will be carried out on children and young adults under the age of 18 if they are symptom-free.
After examination by a neurologist, who will give the patient information about CADASIL, the patient will have an interview with a psychologist and a consultation with a geneticist.
Since the decision on whether or not to use this presymptomatic test is a complex and difficult one, the person concerned must be given the best possible information and support. The psychologist will assess the patient's psychological condition, his or her current thinking and questions about the disease, and his or her ability to deal with a difficult diagnosis. The geneticist will explain the test and the meaning of the results.
If the person decides to have the test, a cooling-off period of one or two months is required before the blood test. It is possible to change one's mind at any time and choose not to know the result. Medical and psychological support is always proposed once the results become available (approximately 3 months after the blood test), whether positive or negative.
Is prenatal or pre-implant diagnosis possible?
In families in which the disease takes a particularly severe form, people do sometimes seek prenatal diagnosis.
The aim of prenatal diagnosis is to determine, during the pregnancy, whether the future child will carry the mutation and therefore develop the disease when an adult (in this case, the parents can request a termination of pregnancy). A prenatal diagnosis is done by sampling the fluid in which the foetus lives (the procedure is called an amniocentesis) or by removing a fragment of placenta (sampling of chorionic villus).
It is also possible to undertake a pre-implant diagnosis (PID), which consists of seeking the genetic abnormality responsible for the disease in the embryos obtained by in vitro fertilisation (IVF). This technique allows the practitioner to select the embryos which are free of the genetic abnormality before implanting them in the uterus, avoiding the parental trauma of a late-term interruption of pregnancy.
Although both prenatal diagnosis and PID are technically feasible, it is nevertheless exceptional to have recourse to them. CADASIL is a disease which only becomes apparent in adulthood and its severity varies from one patient to another, even within a single family. This means that, even is some members of the family are or have been severely affected when they were relatively young, there is nothing to indicate that future children will, if they carry the abnormal gene, have severe symptoms as early in life.
Such an approach to the disease is a very long process, requiring support from the entire care team.
Treatment, care and prevention
Is there any treatment for this disease? What benefits can be expected from treatment?
At present, there is no treatment that can cure the disease or prevent its onset. However, it is possible to treat the symptoms as they occur, to improve the patient's quality of life. Research is underway to identify treatments that might delay the onset of the disease.
Treatment for migraine
Traditional analgesics (pain relief) such as paracetamol, ibuprofen and aspirin (non-steroidal anti-inflammatories or NSAIDs) are used to treat migraine. However, they are often insufficient.
The medicines most commonly used to treat migraine, the so-called "vasoconstrictors or triptan", are not recommended for patients with CADASIL because they cause the blood vessels to contract and may therefore reduce the blood flow to the brain.
Treatment for brain infarction
Aspirin is traditionally used as preventive treatment after the first stroke has occurred. Aspirin increases the fluidity of the blood and limits the formation of the clots that cause most strokes occurring in the population at large. However, in CADASIL patients, the beneficial effects of aspirin have not been clearly demonstrated. If in doubt, most doctors will nevertheless prescribe this treatment, varying the dose depending on the patient, unless there is some contra-indication (stomach ulcer, allergy etc.).
Treatment for alterations
Psychiatric disorders which may produce signs of depression or bipolar disease can be treated with antidepressants but sometimes they may be inadequate or totally ineffective.
What are the other therapeutic options?
After a stroke, physiotherapy is essential to deal with the possible resultant motor disorders (walking, balance etc.). If there are speech difficulties, speech therapy is recommended. If the stroke leaves significant relapse (e.g. paralysis), psychomotricity and ergotherapy can assist the patient by helping him or her to manage his or her handicap and accepting body image so that he or she can develop their maximum potential within their specific environment.
As to treatment for cognitive difficulties, it can include participation in appropriate groups (with other sufferers, for example) to stimulate the patient, avoid isolation and limit the feeling of being a burden on the family or carriers.
If there is a loss of independence (intellectual impairment, behavioral difficulties, significant motor difficulties), the patient may require specialist home care or may even need hospitalisation in a specialist centre where he or she will receive assistance with everyday life (hygiene, diet).
Is psychological support a good thing?
Psychological support is often essential, at every stage of the disease, for both patient and family.
Receiving the diagnosis is a difficult time, often met with a combination of injustice, powerlessness and despair because this is not a treatable disease and it is therefore impossible to foresee how it will develop. In the more or less long term, however, it will cause physical and mental decline.
Moreover, since it is a familial disease, the fear of transmitting (or having transmitted) it to one's children is often strong and associated with a feeling of guilt. Psychological support can help patients to accept the situation more easily and even manage the anxiety linked to the disease more effectively.
For the family (siblings, children), psychological support is important and is helping them reach a decision on whether to ask for a screening test or live with uncertainty without giving up any of their plans for the future. For people who know they are affected but have not yet developed any symptoms, or for the members of the family who do not know whether or not they carry the abnormal gene, it is "natural" to worry at the least neurological sign (headache, pins and needles in a limb etc.). However, CADASIL is not necessarily the cause and two people with the same genetic abnormality will not necessarily have the same symptoms. Nor with the disease develop in the same way. The assistance of a psychologist, in addition to various relaxation methods, can be useful in calming anxiety and fear.
What can one do to help oneself?
There are no particular recommendations but it is preferable to have a healthy lifestyle and to avoid smoking (because it increases the stroke risk). It is also recommended to have regular blood pressure checks.
Generally speaking, to avoid taking unnecessary risks, hormone replacement therapy is only continued at menopause if it brings real benefits (as treatment for hot flushes etc.) and then only for a limited time. As to contraception, a pill containing only progesterone (and without oestrogen) may be preferable to the usual contraceptive pill.
How can the condition be monitored?
CADASIL patients are monitored through specialist consultations in hospital neurology departments. In France, there is one reference centre for rare vascular diseases of the central nervous system (details can be found on the following website www.orphanet.fr). The frequency of consultations and tests will be decided by the medical team.
Certain symptoms should nevertheless ring warning bells in the patient and his family or carers and cause them to seek an urgent appointment. A stroke may lead to difficulties with vision or speech, sudden difficulty in moving a limb (for example, it may become difficult to write), difficulty in coordinating movements etc. Likewise, if there are severe headaches with or without aura, or epileptic seizures, an appointment with the doctor should be sought without delay.
What information is required or should be given to medical teams if an emergency occurs?
In case of emergency, it is important to tell the doctors of the CADASIL diagnosis so that certain treatments or tests can be avoided. For example, anticlotting medication, which is sometimes given after a stroke, is strongly inadvisable for CADASIL patients because of the risk of bleeding in the brain. Likewise, cerebral conventional angiographies (examinations which show blood flow through the arteries in the brain) should be avoided because they may cause a migraine which, in some cases, is very serious. Finally, you must tell the medical teams about current medication and the corresponding doses. This is a precaution, avoiding the combination of incompatible medication and any risk of overdose.
Can the disease be prevented?
To date, nothing has been shown to be effective in preventing the onset or signs of CADASIL.
Living with the disease
What are the consequences of the disease for family, professional, social, educational or active lives?
Suffering from a disease that develops and that, sooner or later, causes physical and mental decline is extremely difficult, even though it is impossible to forecast the severity of the handicap and the speed with which the disease will develop since they vary from one person to another. The neurological problems eventually impair essential functions such as walking or speaking and are, therefore, very disabling. The patient's condition may remain stable for some time but the development of the disease during active life may require the patient to give up work or, at the very least, to redirect or reorganise his or her working life. Moreover, if a stroke occurs, hospitalisation and often lengthy physiotherapy are essential if the patient is to recover as many of his or her faculties as possible.
For people who already have symptoms and for those who know (or think) that they are carrying the disease, the feeling of living under a permanent threat can be difficult to manage and cause immense anxiety. The unforeseeable nature of the disease is particularly difficult to accept.
When the disease is very far advanced, the patient gradually loses his or her independence and becomes incapable of undertaking everyday tasks (washing, eating etc.). For the patient's family or carers, mood disturbances and psychological disorders sometimes accompanied by motor difficulties and incontinence are very difficult to cope with. They often lead to social isolation since friends and, in some cases, family do not always understand the changes in the patient's behaviour. Once the patient become incapable of taking decisions, he or she may have to be placed under guardianship . The guardian, who is often a member of the family, must take responsibility for financial management in the patient's place.
At an advanced stage of the illness, to lighten the burden of maintaining the patient at home, external agencies (home nurses, home carers, cleaning ladies or placement in a specialist home) can be arranged. This "rest" periods are essential for the family.
Pregnancy
It is possible to have children when affected by CADASIL or when one is a carrier of the genetic anomaly responsible for the disease. Pregnancy does not appear to increase the risk of stroke; nor does it cause symptoms in women who have never previously had any signs of the disease.
However, during the month following the birth, the risk of severe migraine with aura would seem to be increased. It is therefore important to discuss any desire for pregnancy with one's doctor or let him or her know if pregnant. This will enable the practitioner to assess the risks for the woman and the future baby and provide the appropriate follow-up.
For further information
What is the current state of research?
The aim of research is to pinpoint the mechanisms through which the anomaly in the Notch3 gene leads to lesions in cerebral arteries. To do this, mice have been produced with an anomaly on the Notch3 gene. The factors determining the severity of the symptoms and the progress of the disease, both of which vary from one patient to another, are also being studied at the present time.
Therapeutic studies are envisaged in the clinical context, in particular to assess the efficacy of vasodilator or neuroprotector medication.
The research is being carried out by various teams worldwide.
How can I contact other patients with the same disease?
By contacting patient associations focussing on this disease. You can obtain their contact details by phoning Maladies Rares Info Services on 08 10 63 19 20 (cost of a local call) or by logging onto Orphanet (www.orphanet.fr)
Social services in France
It is important to find the right people to help you with administrative formalities. Invaluable advice can be gained from social workers in hospitals and from patients' associations which have extensive knowledge of the law and your rights. Moreover, the regional assistance and information departments (SRAI, Services Régionaux d’Aides et d’Informations) in France can help and support families with their everyday requirements by putting them in contact technical staff trained to help the patient back into the workplace (physiotherapists, ergotherapists, social workers etc.).
In France, the medical expenses (i.e. the "co-payment" or "gap") of certain CADASIL patients are fully covered by the Social Security Department. Physiotherapy and speech therapy sessions are paid for by the Social Security Department. Patients may obtain a disabled adult's allowance by applying to their "county" disabled persons' centre (MDPH, Maison Départementale des Personnes Handicapées). Depending on their condition, a disability compensation payment may also be made to patients. Finally, an invalidity card gives disabled adults and children with a disability of more than 80%, certain advantages as regards taxation and transport costs. The "Standing Difficulty" card and the car sticker enable patients to park in places reserved for the disabled. The card and sticker are allocated depending on the condition of the patient. It may be decided by the Committee for the Rights and Independence of the Disabled (CDAPH, Commission des Droits et de l’Autonomie des Personnes Handicapées) to direct patients towards specialist centres.
For further information, check the Orphanet brochure entitled, "Vivre avec une maladie rare en France : aides et prestations" (Living with a rare disease in France: assistance and payments") which compiles all the information on current legislation, assistance, schooling and vocational training available for people suffering from rare diseases.