Definition
Arterio-venous retinal communications are abnormal anastomoses between a vein and a retinal artery. These anastomoses may or may not include an interposed capillary network.
The lesions are classified in 3 groups:
- Group I: anastomosis between a vein and an artery with an interposed network of dilated capillaries. The arteries and veins in a small area of the fundus have lost their normal interdigitation and form a fan-shaped network joined by a few capillaries. These lesions are known as racemose aneurysms.
- Group II: direct anastomosis between a vein and an artery with no interposed capillary network.
- Group III: multiple large arterio-venous anastomoses. It is difficult, in these types, to distinguish the veins from the arteries because the retinal vascular network is totally disordered. These lesions are also known as circoid aneurysms.
Groups II and III may be associated with cerebral vascular abnormalities. This is known as the Bonnet-Dechaume-Blanc or Wyburn-Mason syndrome.
Epidemiology
The frequency of these abnormalities in the general population remains unknown.
Genetics
Arterio-venous retinal communications appear to be congenital abnormalities. To date, no hereditary factor has been identified to explain these lesions.
Diagnosis
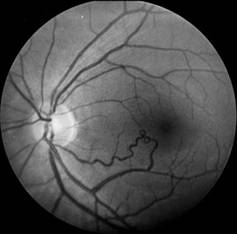
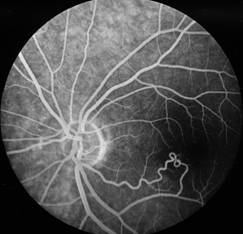
Fig 2 : direct communication between an artery and a retinal vein, with no interposition of capillaries. This is therefore a Group II arterio-venous communication. It is even more clearly visible on the fluorescein angiography (right).
In the Bonnet-Blanc-Dechaume (or Wyburn-Mason) syndrome, there may be vascular malformations in the brain and jaw. A number of cases of dermal angiomas have also been described.
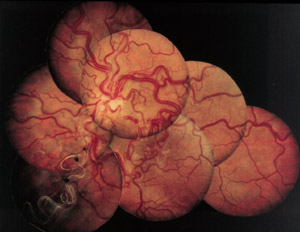
Fig 3 : Complete disorganisation of the retinal vascular network (Group III). The lesions are spread over the whole of the retinal periphery.
Evolution
- Group I: the lesions are usually stable and visual acuity is maintained.
- Groups II and III: the patient may experience some loss of vision as the disease develops. This may be secondary to an arterial or venous occlusion, macular oedema or serous retinal detachment of the macula, an intravitreous haemorrhage or gradual compression of the optic nerve.
Treatment
There is no treatment to re-establish a normal vascular path. In patients in Groups II and III with severe loss of vision as a result of serous retinal detachment of the macula or a spread through the communication, laser photocoagulation may be offered. Vascular occlusions usually resolve spontaneously. Laser photocoagulation will only be proposed for patients with vascular occlusion leading to extensive retinal ischaemia. Haemorrhages of the vitreous persisting for more than 3 months are treated by vitrectomy.